SEARCH OUR WEBSITE
If you are diagnosed with skin cancer, there are several treatment options that may be available to you depending on the type of cancer, location on the body, and extent of the damage. At Dermatology + Plastic Surgery, led by board-certified dermatologist Anita Saluja, MD and double board-certified plastic surgeon Rebecca Novo, MD, the best treatment options and precise surgery for skin cancer are helping residents of Melbourne, Indialantic, Viera, Brevard County, the beaches, and nearby communities in the Central Florida area live healthy, cancer-free lives.
SURGERY FOR BASAL AND SQUAMOUS CELL SKIN CANCERS AND MELANOMA
Surgery is the most common and effective treatment for skin cancers. Different surgical techniques may be applied, depending on the type of skin cancer, its size and location on the body, how early or advanced the cancer is, and other factors. The surgery is typically performed as an outpatient procedure using local anesthesia and postoperatively, pain is usually nonexistent or minimal. If you desire a relaxing medication or pain medication ahead of time, please call the office to discuss. If you are taking blood-thinning medication or supplements, please discuss your individual situation with us for our recommendations. When treating more aggressive or advanced cases of skin cancer, surgery may be combined with other treatments, such as chemotherapy or radiation. If another specialist needs to be consulted, you will be assisted in this aspect.
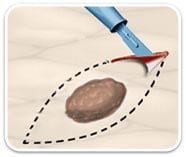
EXCISION SURGERY
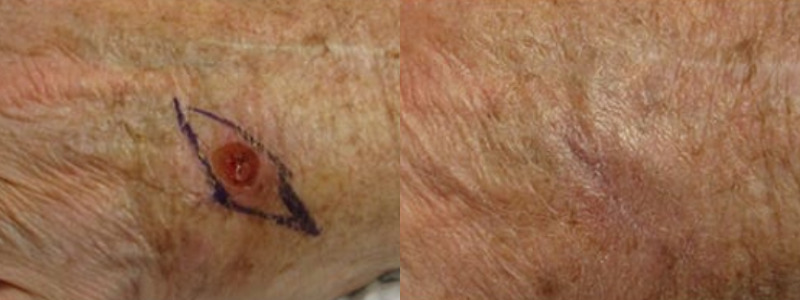
Excision surgery is basically the same procedure used to collect skin cells for a biopsy performed until all malignant cells are removed from the site. A local anesthetic is administered, and the malignant growth is removed using a surgical scalpel. In most cases, some surrounding normal skin cells are also removed with the tumor for a margin of safety. The specimen is examined by the pathologist to check for clear deep and peripheral margins. After careful suturing, this procedure typically leaves a fine line scar on the skin.
FROZEN SECTION SURGERY OR MOHS SURGERY (MICROSCOPICALLY CONTROLLED SURGERY)
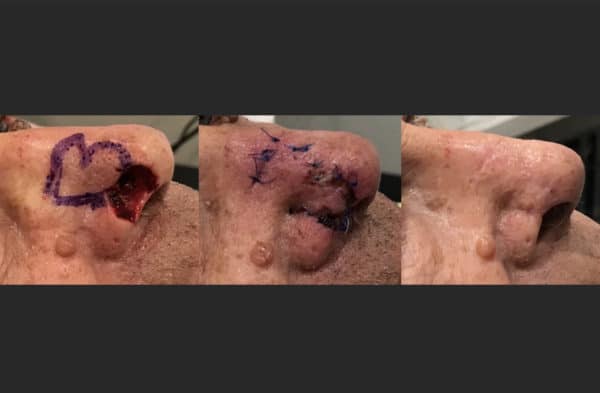
Surgeons require special training to perform frozen section surgery or Mohs surgery (microscopically controlled surgery). In this procedure, a very thin layer of the skin, including the tumor, is removed and examined under a microscope. If cancer cells are detected, another layer is removed and examined, and so on until all of the malignant cells are removed. This procedure is time-consuming and may take several hours to perform, but it allows for more normal skin cells in the area surrounding the tumor to be saved. The decision to use frozen section surgery or Mohs surgery typically depends on the type of skin cancer, its size and location of the body, and other factors. Not all skin cancer warrants this type of surgery and we will follow the current guidelines of care in helping determine the best treatment and discussing this with you. Frozen section surgery or Mohs surgery is the procedure of choice in cases where there is a high probability that the cancer will return after treatment, in cases where usual margins of safety cannot be taken, or in cases where the extent of the cancer is difficult to determine. It may also be used when removing tumors near the eye or other critical areas. In frozen section surgery, the removed tissue is frozen and examined underneath the microscope while you wait. Further tissue is removed as warranted to clear margins before the skin is reconstructed and repaired.
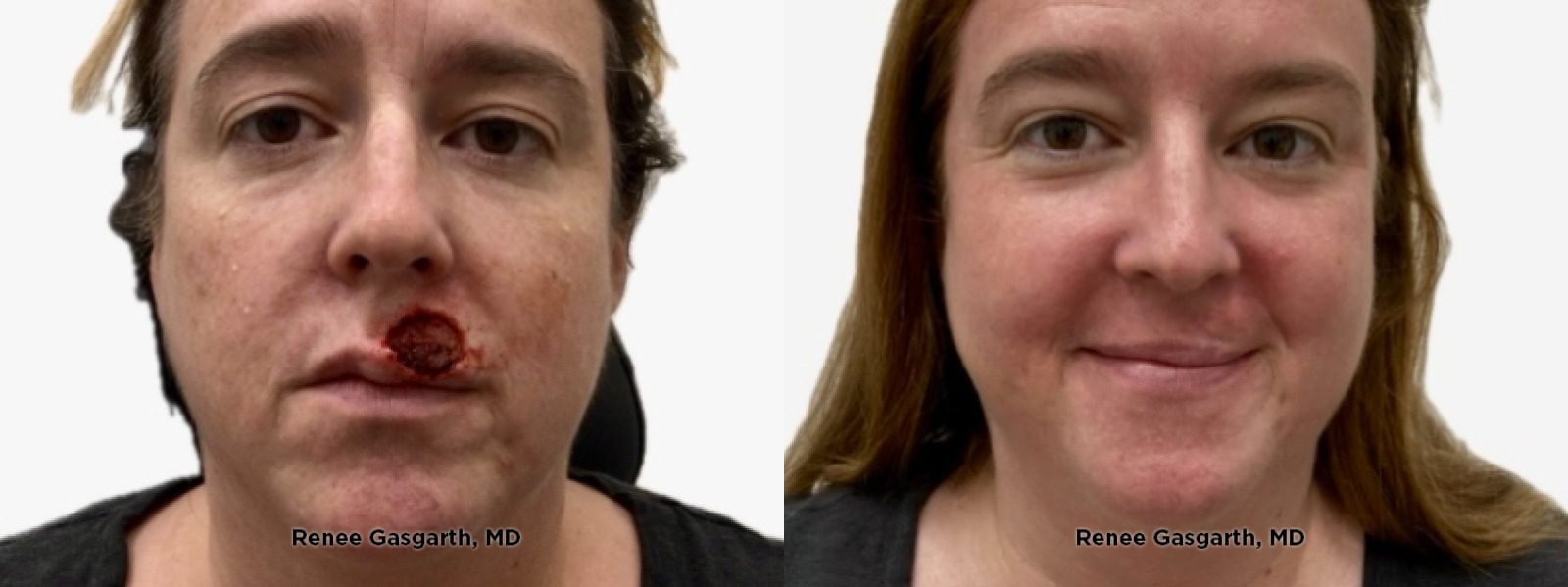
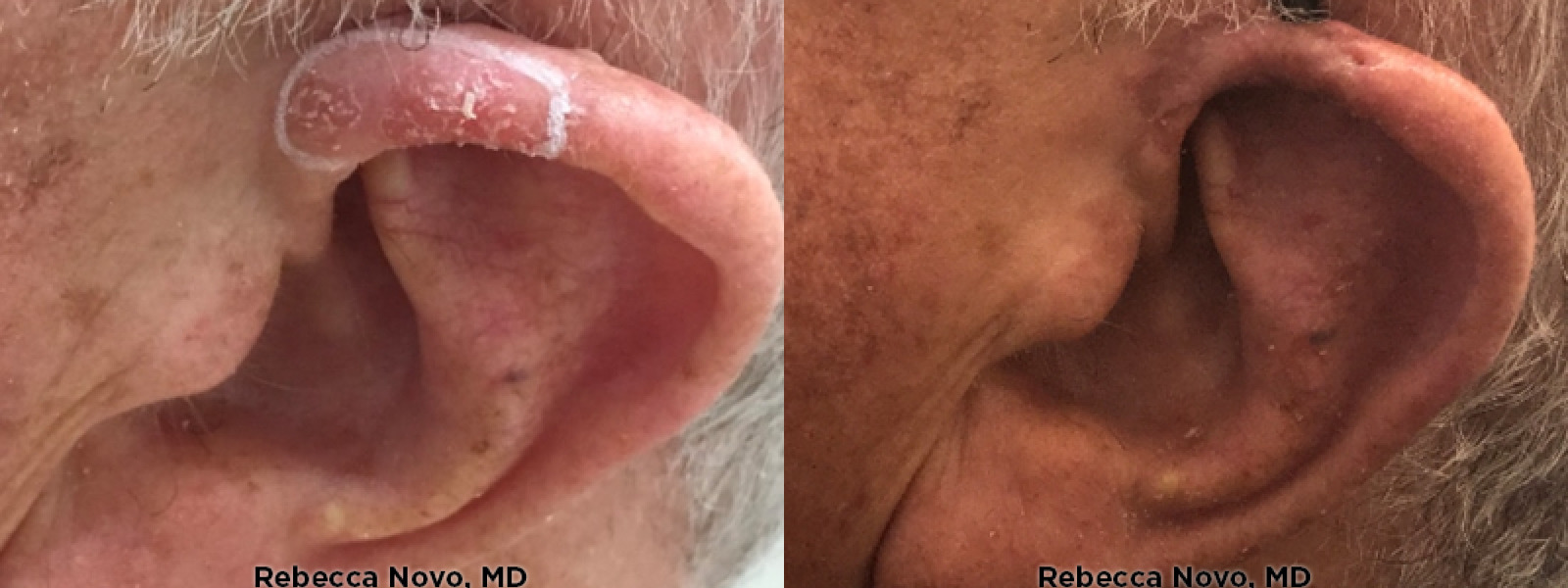
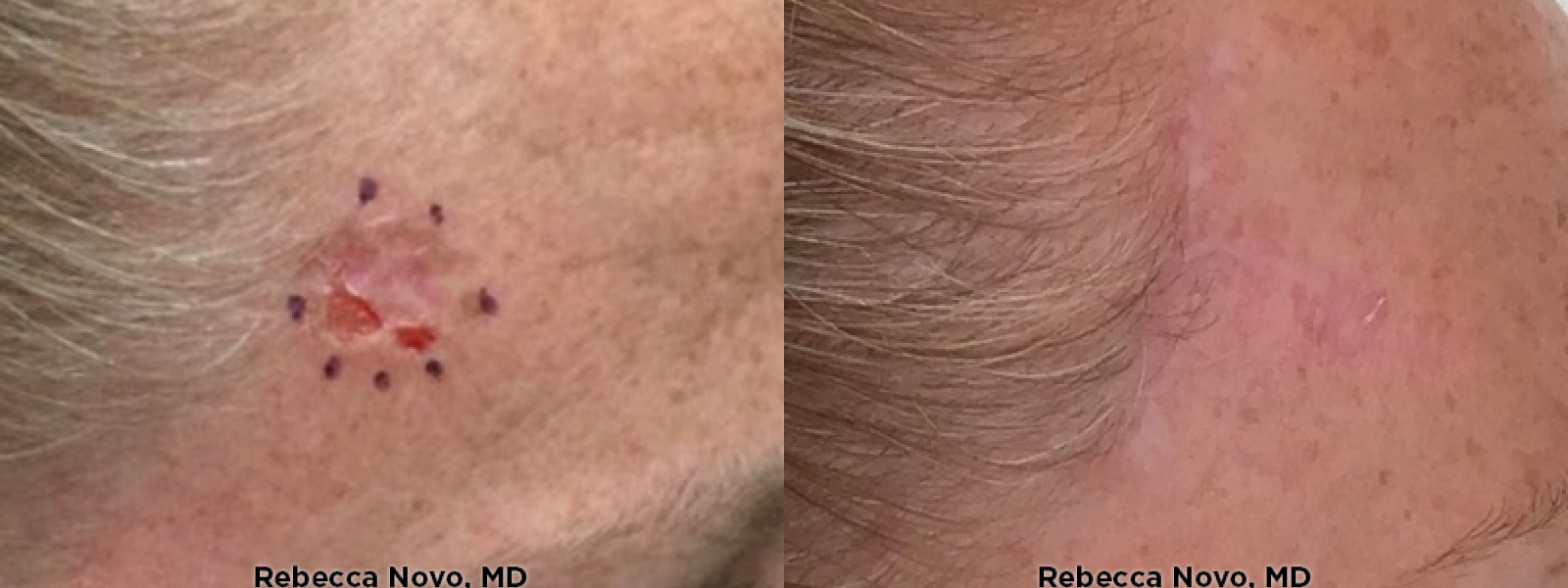
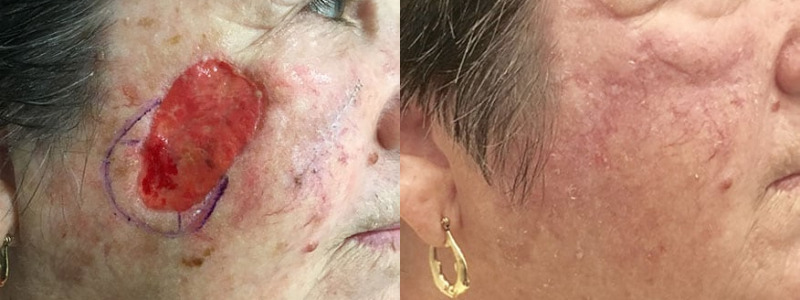
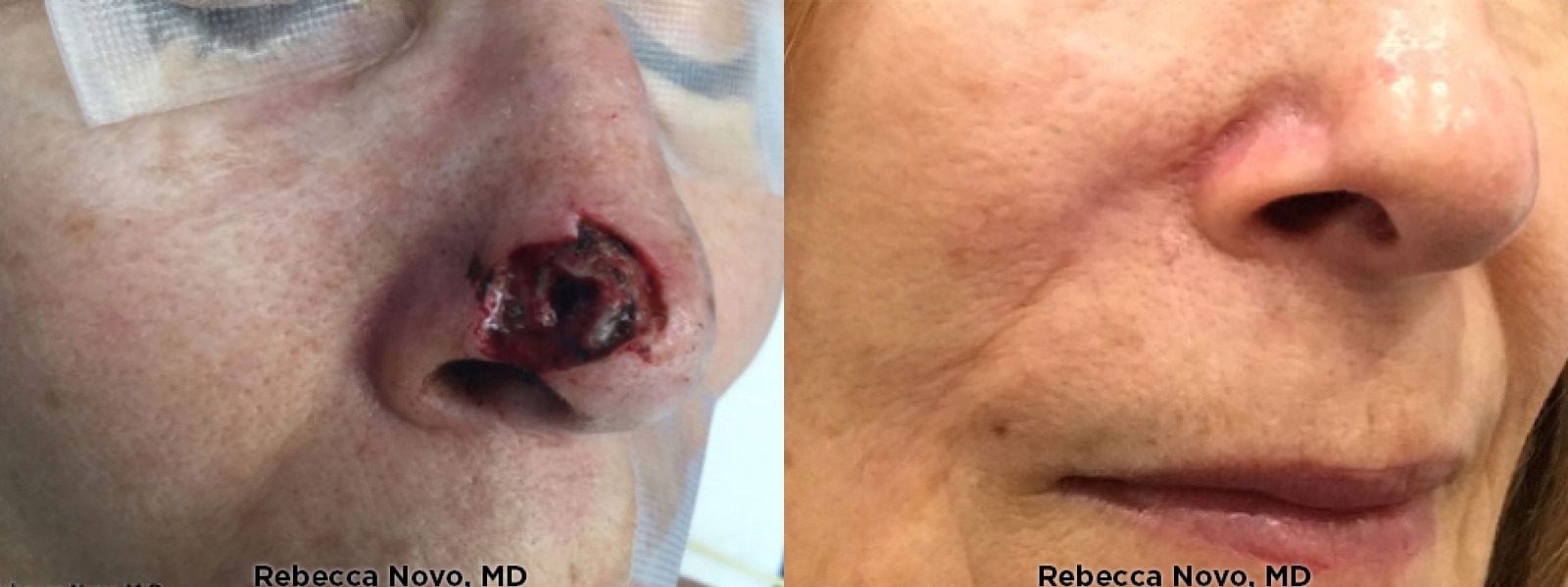
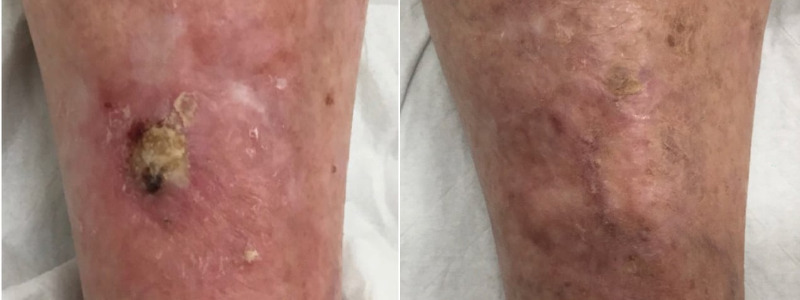
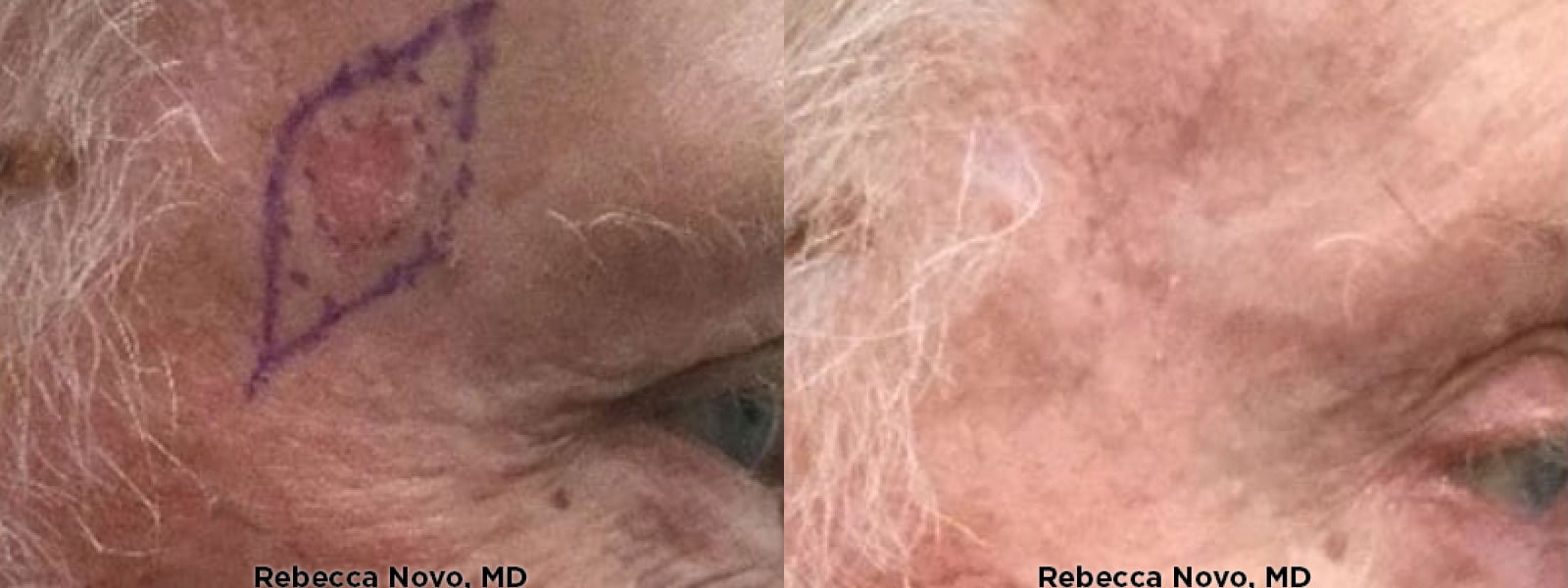
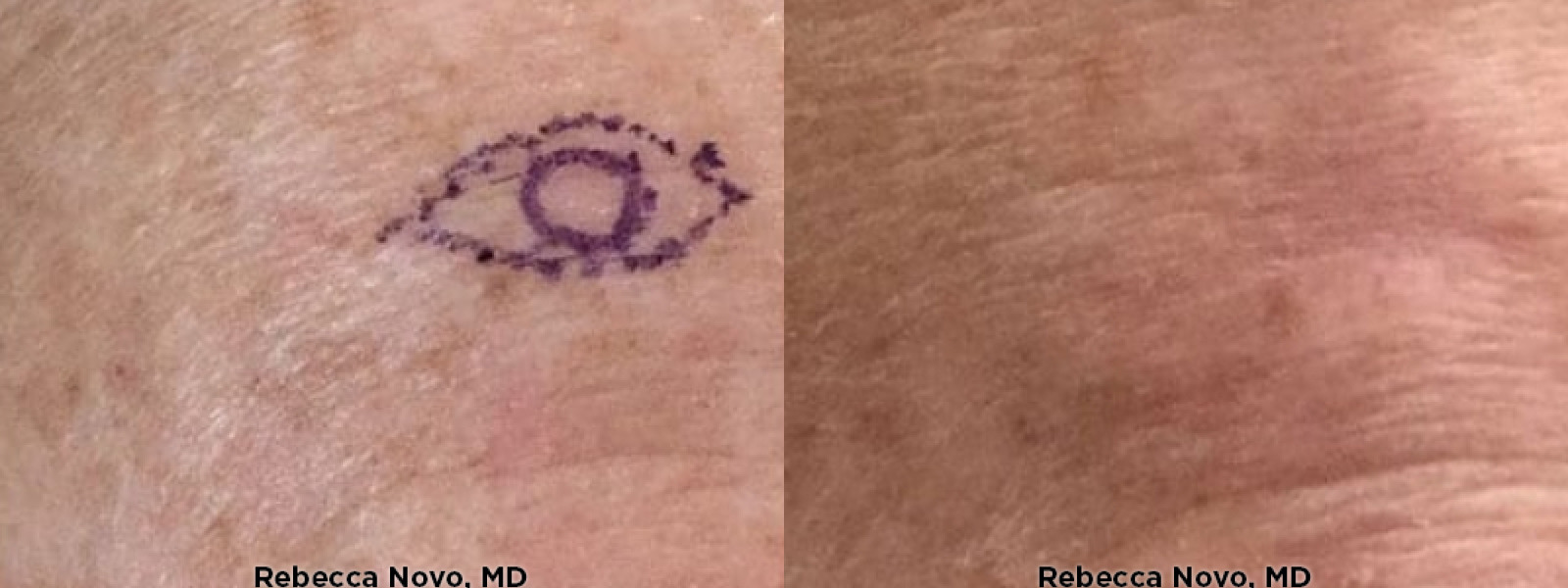
NATURAL, AUTHENTIC Results
VIEW GALLERYCURETTAGE AND ELECTRODESICCATION & CURETTAGE AND CRYOSURGERY
Curettage and electrodesiccation or curettage and cryosurgery are generally recommended to remove superficial non-melanoma skin cancer such as superficial basal cell carcinoma and squamous cell carcinoma in situ that is confined to the outermost layers of skin. This procedure removes the cancer using a long, thin utensil called a curette that has a sharp looped edge on one end used to gently scrape off malignant skin cells. An electric needle (electrode) or liquid nitrogen is then applied to destroy any remaining cancer cells. This process may be repeated during the same office visit. It will most often leave a light or white colored or brown scar. Scars take 6-12 months to naturally improve, and patients are often pleasantly surprised what time will do for scars. To reduce the appearance of scars, click here to learn more from Dr. Saluja.
CRYOSURGERY
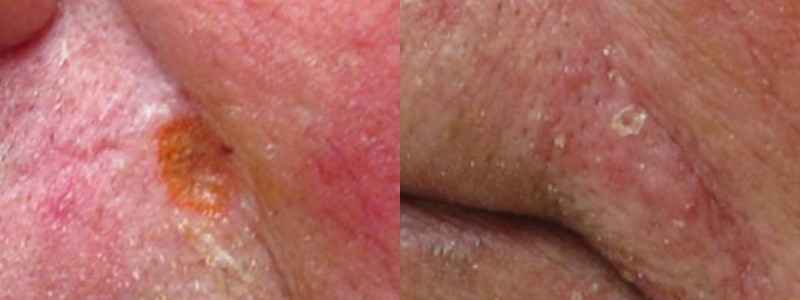
Cryosurgery removes premalignant actinic keratoses and superficial malignant tissue (superficial basal cell carcinoma) by freezing it. It can also be used for benign lesions such as warts or skin tags. Liquid nitrogen is applied to the lesion using a spray device. Cryosurgery requires no cutting or scraping. Following the treatment, the treated area may blister or form a scab and fall off naturally, usually within a few weeks. The procedure may cause temporary redness and swelling, and in some patients, loss of pigment at the site. This procedure is especially recommended for patients with bleeding disorders or those who cannot tolerate anesthesia. Although cryosurgery is safe and convenient, it is used less frequently than other treatments because it has a cure rate of about 85 to 90 percent, while surgical or combination curettage plus cryosurgery techniques have higher successful cure rates.
Cryosurgery Aftercare Instructions: No special care is needed after liquid nitrogen treatment. You can wash and take care of your skin as usual. It is ok to apply petrolatum jelly, antibiotic ointment, or scar gel, or to cover with a bandaid if you prefer. Freezing peels off the lesion, replacing it with new skin in about 10-14 days. A blister or scab often forms within the first few days. There may also be some redness and mild discomfort at the treated site. If you experience increasing redness, warmth, or pain, or have other concerns, call our office. If any of the treated lesions persist or recur, it is important to return for re-evaluation and further treatment because sometimes, a skin biopsy for further diagnosis or two or more rounds of freezing treatment are needed.
PHOTODYNAMIC THERAPY (PDT)
PDT is an FDA-approved procedure to treat actinic keratoses and, more rarely, superficial basal cell carcinoma, with a 70- to 90 percent cure rate. This procedure works by applying a light-sensitizing agent called Levulan directly onto the tumor. The treated area is then activated using a strong blue light. The blue light will selectively destroy malignant cells while leaving the surrounding normal tissue unaffected. The procedure may cause some redness, pain, and swelling, and it is imperative for patients to avoid sunlight for at least 48 hours to prevent UV exposure that may further activate the medication, causing severe sunburn and skin damage. For more information on Levulan – BluU, click here.
LASER SURGERY
In laser surgery, a laser may be used to vaporize or ablate the top layer of skin to destroy pre-malignant cells. This procedure has been used effectively to treat actinic keratoses. Although laser surgery is yet to be FDA-approved as a treatment for basal cell carcinoma, it is sometimes used as a backup treatment for small, superficial basal cell carcinomas when other techniques are not options or prove unsuccessful.
SKIN GRAFTING AND RECONSTRUCTIVE SURGERY
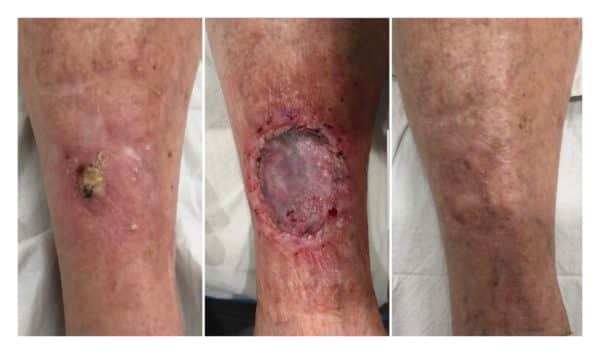
Skin grafting involves the transplantation of skin cells to repair an area damaged by cancer or cancer treatment. Skin grafting may reduce the course of treatment needed, and it may also improve the function and appearance of the treated area. Many patients opt for skin grafting surgery following skin cancer treatment.
To reduce the appearance of scars, Dr. Saluja provides information on how to make them look better.
Safe, individualized, and comprehensive skin cancer surgery with cancer cure and cosmetic outcome top of mind is provided at Dermatology + Plastic Surgery, led by board-certified dermatologist Anita Saluja, MD and double board-certified plastic surgeon Rebecca Novo, MD, and serving residents of Melbourne, Indialantic, Viera, Brevard County, the beaches, and neighboring areas in Central Florida. Contact our office today to learn more about skin cancer surgery and treatment options.
Click here to learn more about our new medical dermatology practice, explore our comprehensive services and connect with our expert medical team.
CREATING LIFELONG RELATIONSHIPS With Our Patients
READ MORE REVIEWSCONTACT US / REQUEST APPOINTMENT
Fill out the form below or call us at (321) 395-3298 to schedule your appointment or consultation.
OUR BLOG
Learn More
REVEAL YOUR MOST Radiant Skin
Dermatologist Dr. Anita Saluja and plastic surgeon Dr. Rebecca Novo have created an online shop for your convenience. They have curated scientific skin care products that they believe will deliver results: For Your Best Self. And you can always contact our office with any questions.
SHOP OUR SKIN STORE