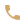SEARCH OUR WEBSITE
If you have dry, scaly patches or unusual “sandpapery” spots on your skin, these may be actinic keratoses, or precancerous growths that are common among adults with a history of excessive sun exposure. At Dermatology + Plastic Surgery, led by board-certified dermatologist Anita Saluja, MD and double board-certified plastic surgeon Rebecca Novo, MD, residents of Melbourne, Indialantic, Viera, Brevard County, the beaches, and nearby communities in Central Florida can obtain early treatment for actinic keratosis before it becomes something worse.
What does Actinic Keratosis look like?
Actinic keratoses (AKs for short), or solar keratoses, develop after repeated exposure to the sun. Your skin “remembers” all the sun damage it has had since you were a child including sunbathing, playtime, yard work, vacations, sporting activities, and sunlight that hit your skin going to and from your normal daily activities. AKs are scaly or crusty spots on the skin that may be tan, pink, or red. They feel rough and are often easier felt than seen. They may itch or be prickly or feel tender. Vulnerable areas are the face, lips, ears, and the back of the neck or hands.
Why is it important to treat Actinic Keratosis?
Actinic keratosis can progress into squamous cell carcinoma, so it is important to treat actinic keratosis before it progresses.
Who is most likely to develop Actinic Keratosis?
The condition develops over many years of sun exposure, so it is usually most often found in adults over the age of 40. People who are exposed to excessive amounts of sunlight due to lifestyle or geographical location are at greatest risk. The incidence is higher in regions closer to the equator and slightly higher among men who tend to use less sun protection and spend more time in the sun practicing sports or performing jobs that require being outdoors. People of all ethnic groups can get actinic keratosis, but it is most common in fair-skinned people with light eyes.
How is Actinic Keratosis treated?
Actinic keratosis may be removed much like skin cancer tumors using various techniques, including cryosurgery, excision, curettage and electrodesiccation, photodynamic therapy (PDT), or laser treatments.
Cryosurgery or freezing is the most common method of treatment. This is only uncomfortable for a few minutes and causes the skin to separate between normal skin and the actinic keratosis. The AK will peel off when the skin underneath is healed. This can take 10-14 days.
Topical prescription medication is also an option especially if there are extensive AKs. Ingredients include fluorouracil, imiquimod, diclofenac, and ingenol. The skin may become red and raw.
Photodynamic therapy (PDT) includes the use of Levulan, a solution that incubates on the skin, and then, a blue light source is used to activite it, removing AKs over a few weeks.
There are also in-office laser treatments we do to treat AKs, as well as cosmetic concerns. Many of our patients return to the office annually for a laser skin peel.
Helpful Hints When Using Actinic Keratosis Medication:
- Do not use if you are pregnant or nursing.
- Inform us if you have a history of cold sores or fever blisters if you are using medication on your lips or face.
- Apply only a small amount to the affected area – you do not need to apply thickly.
- It is normal for there to be irritation (redness and peeling) and mild discomfort with the medication. If it becomes bothersome, discontinue the cream for 3-4 days, and then attempt to restart.
- Call the office and stop the medication if there is severe pain or severe irritation (such as crusting, bleeding, or sores).
- Use the prescribed ointment (best for healing), over the counter 1% hydrocortisone ointment, or Aquaphor healing ointment once irritation is significant and for a few weeks after treatment is over to help decrease irritation more rapidly.
- It is good to protect the skin from the sun as much as possible during treatment and healing. It is ok to use sunblock, moisturizers, and makeup if they don’t sting. Hold on any anti-aging retinols or hydroxy acids.
- Redness dramatically improves over a few weeks but may take a few months or more to fully fade.
- Thoroughly wash hands after use of medication, medication left on fingers can inadvertently treat other areas or cause discomfort if touching sensitive areas after application.
Call the office if any lesions (pink dry or scaly areas or bumps) persist after the skin has healed from the medication reaction. Healing usually takes 2-3 weeks.
What is Seborrheic Keratosis?
Seborrheic keratoses (SKs) are benign lesions that are not precancerous or cancerous. They tend to start appearing in adulthood and usually increase in number over time. SKs are not related to sun exposure. They tend to run in families.
SKs are usually slightly raised, light to tan to dark brown bumps. They are usually rough, scaly, crusty, or warty in appearance. They can increase in size or number. SKs tend to be “stuck on” the skin and many people scratch them off accidentally and harmlessly.
SKs cannot be prevented from appearing. They do not need to be treated. They are often treated due to symptoms or due to cosmetic appearance. Treatment is minimally invasive and comfortable. SKs are frozen off with liquid nitrogen, shaved off with a blade, desiccated off with an electric tip, or scraped off with a curette.
Does health insurance cover Actinic keratosis treatment?
Your health insurance may cover part or all of the cost for treatment of actinic keratosis. To help patients manage costs not covered by health insurance, our office provides various payment options.
It’s better to be safe than sorry, especially where your health is concerned. If you have unusual spots that may be actinic keratosis, visit the team of specialists at Dermatology + Plastic Surgery. Led by board-certified dermatologist Anita Saluja, MD and double board-certified plastic surgeon Rebecca Novo, MD, Dermatology + Plastic Surgery offers actinic keratosis diagnosis and cancer screening to the residents of Melbourne, Indialantic, Viera, Brevard County, the beaches, and nearby communities in Central Florida. Contact our office today to learn more about early treatment options for actinic keratosis and skin cancer screening.
Click here to learn more about our new medical dermatology practice, explore our comprehensive services and connect with our expert medical team.
Frequently Asked Questions
Can actinic keratosis turn into basal cell carcinoma?
Does actinic keratosis need to be removed?
Does hydrocortisone help actinic keratosis?
Can actinic keratosis spread?
Do chemical peels help actinic keratosis?
Does actinic keratosis come back?
Can actinic keratosis turn into cancer?
CREATING LIFELONG RELATIONSHIPS With Our Patients
READ MORE REVIEWSCONTACT US / REQUEST APPOINTMENT
Fill out the form below or call us at (321) 395-3298 to schedule your appointment or consultation.
OUR BLOG
Learn More
REVEAL YOUR MOST Radiant Skin
Dermatologist Dr. Anita Saluja and plastic surgeon Dr. Rebecca Novo have created an online shop for your convenience. They have curated scientific skin care products that they believe will deliver results: For Your Best Self. And you can always contact our office with any questions.
SHOP OUR SKIN STORE